Cookie Bite Hearing Loss: What It Is and How to Manage It
Imagine listening to your favorite song and suddenly the middle notes vanish. That’s what cookie bite hearing loss is like—it makes mid-range sounds, such as certain voices and common noises, tougher to catch.
If you’re living with—or just curious about—cookie bite hearing loss, understanding how it works is important. While it’s not as common as hearing loss caused by aging or loud noise, it brings its own challenges and can have a real impact on how you connect with others.

Where Does “Cookie Bite Hearing Loss” Get Its Name?
The quirky name “cookie bite” comes from how this type of hearing loss appears on an audiogram—a chart that maps out how loud sounds need to be for you to hear them.
On an audiogram for someone with cookie bite hearing loss, you won’t see the line simply sloping up or down as with other types of hearing issues. Instead, there’s a noticeable U-shaped dip in the middle of the chart—almost as if someone took a bite right out of it. That distinctive “bite” is what gives this hearing pattern its name.
Understanding Cookie Bite Hearing Loss
Cookie bite hearing loss is distinctive because it affects the middle frequencies—the “heart” of our hearing range.
People with this condition can often still hear:
- Low-pitched sounds (like distant thunder)
- High-pitched sounds (like birds chirping)
The trouble starts with middle tones, which include much of:
- Speech clarity (especially vowel sounds and certain consonants)
- The core of melodies in music
- Everyday environmental sounds
It’s not just that sounds are softer—voices, music, and daily noises can lose their crispness. Words may seem mumbled or incomplete, making conversations harder to follow, even in quiet rooms.
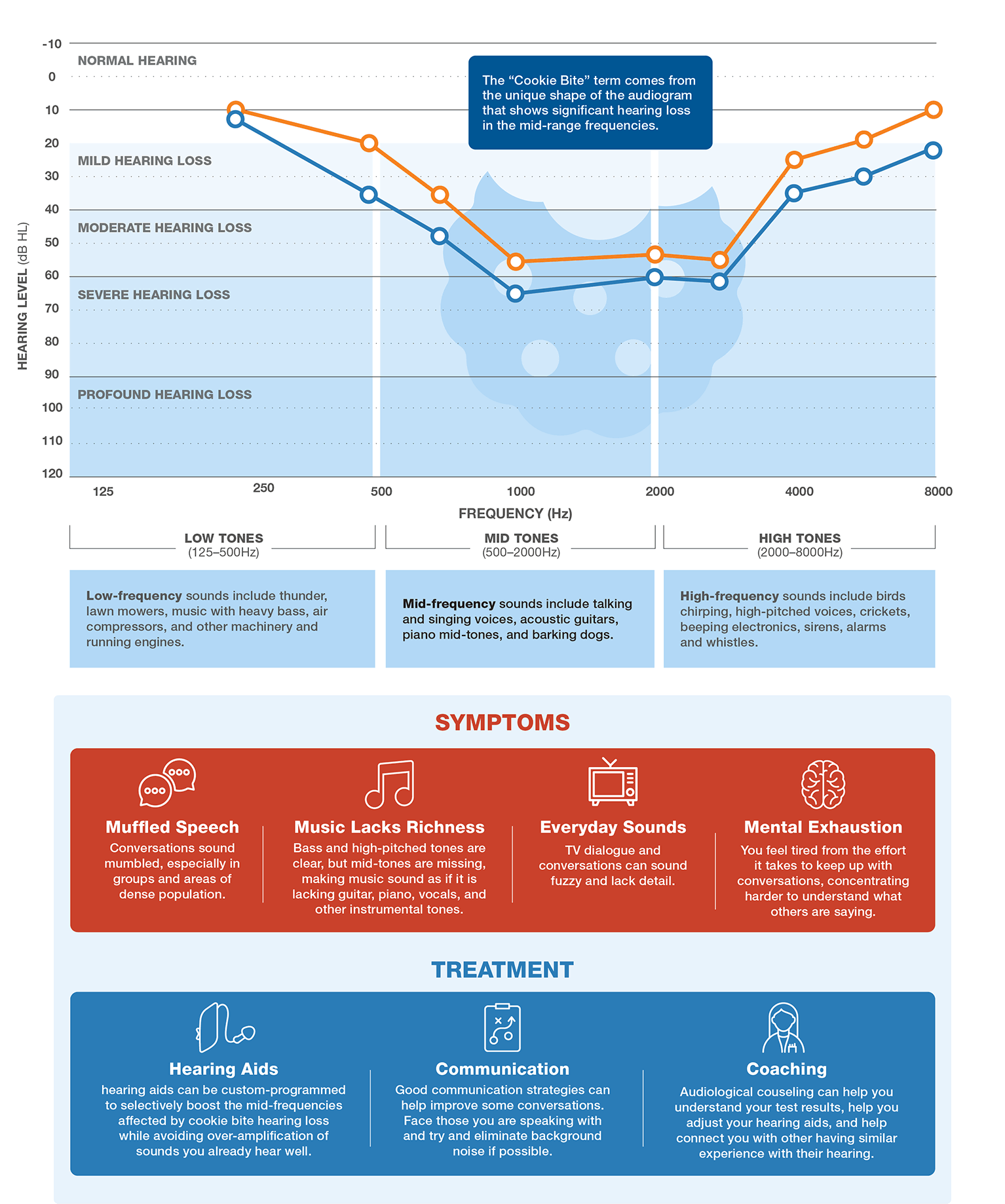
Signs of Cookie Bite Hearing Loss
Unlike patterns of hearing loss that only affect high or low tones, cookie bite hearing loss makes it hard to catch many familiar sounds in everyday conversation and music.
Common signs include:
- Speech sounds muffled or as if everyone is mumbling, especially in groups or busy places.
- You hear deep rumbles and high-pitched sounds, but speech and other mid-tone sounds are harder to catch.
- Music seems less full or rich—the middle of the melody feels like it’s missing, even when bass and high notes come through clearly.
- Everyday sounds like conversations, TV dialogue, or a grandchild’s story seem fuzzy or lacking detail.
- You find yourself asking people to repeat themselves more often, especially during phone calls or family gatherings.
- You feel extra tired from the effort it takes to keep up with conversations, needing to concentrate harder to understand what others are saying.
If the sounds that make life lively and connected are fading or losing their sharpness, it may be a sign of cookie bite hearing loss. Recognizing these early changes is the first step toward rediscovering how vibrant everyday sounds can be—and taking charge of your hearing health.

The Cookie Bite Audiogram: A Distinctive Diagnostic Signature
Think of an audiogram as a visual snapshot of your hearing. During a hearing test, a hearing care professional plays different pitches—from deep bass to high, bird-like chirps—and records the quietest level you can hear at each pitch. These results are plotted on a graph:
- Horizontal axis: Frequency (pitch), from low to high
- Vertical axis: Volume (loudness), from soft at the top to loud at the bottom
With typical hearing, your line on this graph stays fairly flat and close to the top, meaning you pick up a wide range of sounds without much difficulty.
Cookie bite hearing loss looks different. The line dips in the middle but rises again at both ends, forming a U-shape. That “bite” appears because the softest sounds you can hear in the middle frequencies (often between about 500 and 4000 Hz) need to be much louder than very low or very high pitches for you to detect them.

Unraveling the Causes: Genetics and Other Factors
The cause of cookie bite hearing loss is most often genetic. This makes it different from many other types of hearing loss, which are more commonly tied to aging, loud noise, or injury.
The Predominant Role of Genetics
Many people ask, “Is cookie bite hearing loss hereditary?” In most cases, yes.
Most cases are linked to changes in genes that guide how the inner ear—especially the hair cells in the cochlea—develop and function.
For example:
- Mutations in a gene called TECTA are often involved. This gene makes a protein called alpha-tectorin, which helps the ear turn sound waves into signals your brain can understand. If this protein doesn’t work correctly, it can affect how you hear sounds in the middle range.
- Other genes, such as WFS1 and some known as DFNA types, may also play a role.
These gene changes can be passed down in families, which is why you might notice hearing loss running from parent to child or across several generations. In many cases:
- Only one parent needs to carry the gene for it to appear in a child (dominant inheritance), or
- Both parents must carry the gene, even if they don’t have hearing loss themselves (recessive inheritance).
People are often born with cookie bite hearing loss, or it may become noticeable in childhood or early adulthood. How quickly it progresses can vary widely. Because gene involvement can be complex, your provider may ask detailed questions about your family hearing history and, in some cases, recommend genetic counseling.
Less Common or Contributing Factors
While genetics are the main cause, a few other, less common factors may contribute to similar hearing patterns:
- Rare inner-ear abnormalities or certain metabolic disorders.
- Conditions such as Meniere’s disease, which usually affects lower-pitched sounds but can sometimes resemble mid-frequency loss. These often come with additional symptoms (like vertigo) or show different patterns on an audiogram.
- A benign tumor on the hearing nerve, called an acoustic neuroma, can cause hearing changes—though it usually:
- Affects only one ear
- Targets higher pitches
- Is often accompanied by ringing (tinnitus) or balance issues
For most people with this specific “cookie bite” pattern in both ears, genetics are the primary cause. That’s why exploring your family’s hearing history can be so helpful.

Is Cookie Bite Hearing Loss a Disability?
Cookie bite hearing loss is often considered a disability because it can make everyday communication—including group conversations and noisy settings—much more difficult.
Possible impacts include:
- Struggling to follow conversations at work or social events
- Withdrawing from gatherings because listening feels exhausting
- Challenges with school or job performance if instructions are missed
- Increased listening effort, which can contribute to fatigue and reduced concentration
- Associated symptoms like tinnitus (ringing in the ears)
Because of these factors, getting support and appropriate treatment is important—not only for communication, but also for emotional well-being and cognitive health.
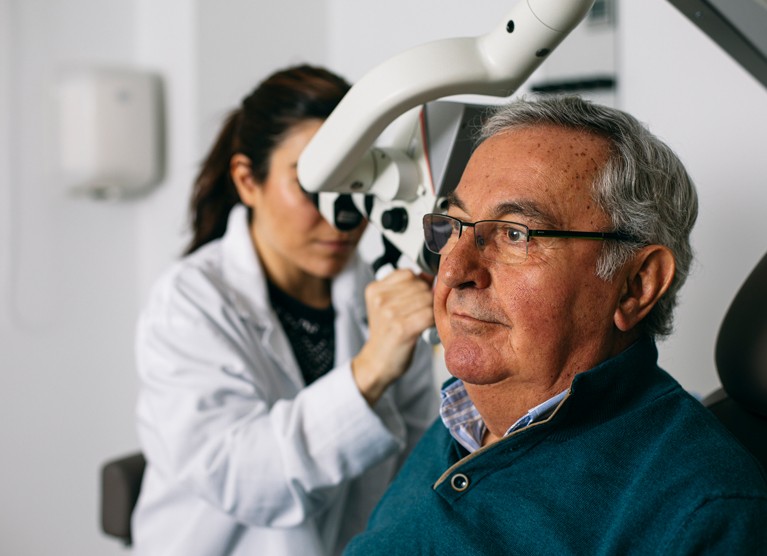
Diagnosing Cookie Bite Hearing Loss: The Path to Clarity
Diagnosing cookie bite hearing loss takes more than simply noticing you’re missing parts of conversations. A hearing care professional will typically follow a step-by-step process:
- Personal conversation: Your hearing care professional will ask about:
- When you first noticed changes in hearing
- Whether hearing issues run in your family
- Which situations are most difficult (e.g., phone calls, group settings, meetings)
- Ear checkup (otoscopy): A quick, gentle look inside your ears to rule out earwax buildup, infection, or other blockages.
- Pure-tone audiometry: You’ll wear headphones and press a button (or raise your hand) when you hear tones at different pitches and volumes. This test produces your audiogram, where cookie bite hearing loss typically shows a U-shaped dip in mid-range tones.
- Speech audiometry: You’ll listen to and repeat words at different volumes. People with cookie bite loss often report that voices are especially hard to understand in background noise, even if sounds aren’t extremely soft.
Each step helps build a detailed picture of your hearing profile so your hearing care professional can recommend the best support.
Effective Management and Treatment Options
While there is currently no “cure” that restores normal hearing in cookie bite hearing loss, there are highly effective ways to improve communication and daily comfort.
Prescription Hearing Aids
Digital hearing aids can be custom-programmed to selectively boost the mid-frequencies affected by cookie bite hearing loss while avoiding over-amplification of sounds you already hear well.
A hearing care professional will fine-tune settings so speech and everyday sounds are clearer but still comfortable and natural.
Common styles include:
- Behind-the-Ear (BTE): Versatile and durable, with components positioned behind the ear.
- Receiver-in-Ear (RIE/RIC): A discreet style that offers a strong balance of comfort, performance, and visibility.
- Completely-in-Canal (CIC) or In-the-Canal (ITC): Custom-molded to fit snugly in the ear canal and designed to be nearly invisible.

Communication Strategies
Simple adjustments can greatly improve day-to-day conversations:
- Ask friends and family to face you and speak clearly at a natural pace.
- Reduce background noise when possible (lower the TV, move away from loud speakers, choose quieter tables in restaurants).
- Use visual cues like facial expressions and lip movements to support understanding.
Coaching and Support
Audiological counseling and support groups can help you:
- Understand your hearing test results
- Adjust to using hearing aids or other technology
- Connect with others who share similar experiences
Emerging treatments like gene or stem cell therapies are still in the research phase and are not part of routine care. For now, partnering with a hearing care professional and using well-fitted hearing technology remains the most effective approach.

Progression and Long-Term Outlook
Is cookie bite hearing loss progressive? It can be—but not always.
Progression varies:
- Some people experience relatively stable hearing over many years.
- Others may notice gradual decline, often starting in the mid-range and sometimes extending into other frequencies.
Because genetics play a major role, some inherited forms stay fairly stable, while others slowly worsen over time.
Staying proactive helps:
- Schedule regular hearing checks to monitor changes.
- Use your hearing aids consistently if they’re recommended.
- Discuss family history and possible genetic counseling with your healthcare provider if hearing loss runs in your family.
Addressing hearing loss early can support brain health, help maintain social connections, and reduce listening fatigue.

Living Well With Cookie Bite Hearing Loss
Living with cookie bite hearing loss can be challenging—but with the right tools and support, you can stay engaged and connected.
Helpful steps include:
- Working with a hearing care professional to find hearing aids matched to your specific hearing pattern.
- Sharing your needs with loved ones so they can support you (for example, by facing you when they speak).
- Using visual cues and strategies in conversations, especially in noisy places.
- Exploring local or online support groups for encouragement and practical tips.
- Staying informed about new hearing technologies and treatment advances.
With tailored hearing solutions, regular follow-up, and supportive communication strategies, it’s possible to continue enjoying conversations, music, and everyday sounds—and to thrive with cookie bite hearing loss.

Take Online Hearing Test
Take our free at-home hearing loss test as a first step on your journey to better hearing.

Book Your Free Appointment

Reviewed By
MJ DeSousa; B.Sc.(H), M.Cl.Sc, Aud(C)
MJ DeSousa is an Audiologist and Director of Patient Experience at Beltone, with over 35 years of experience in hearing health care. She earned her Masters of Clinical Science in Audiology from Western University in London, Ontario and has extensive experience as a practicing Audiologist and in corporate leadership within the hearing industry. At Beltone, DeSousa is dedicated to educating hearing care professionals across North America, ensuring they provide the highest standard of patient care. Learn more by visiting her LinkedIn here.

Reviewed By
Kathy McGowan, AuD CCC-A, Doctor of Audiology
Kathy McGowan is the Manager of Managed Care Programs with Beltone Corporation . Kathy worked with the Professional Development Training Team as well as the Operations Team and Beltone Corporate Retail for 8 years before being promoted to her current position. Prior to joining Beltone Corporate, Kathy worked for 10 years as an Audiology Manager in a private practice. She has worked in many settings as an Audiologist including an ENT practice, a hospital, an Optical and Hearing Company, and in the Military, retiring as a LtCol. Kathy earned her Bachelor’s in Speech and Hearing and Master’s in Audiology from Ohio University in Athens, Ohio, and went on to receive her Audiology Doctorate from A.T. Still University School of Health Sciences. Kathy is currently licensed in seven states.

