Understanding Presbycusis: A Comprehensive Guide to Age-Related Hearing Loss
April 06, 2026 Presbycusis disease is one of the most common conditions affecting older adults worldwide. Despite its prevalence, it’s still widely misunderstood, often leading to unnecessary frustration and social isolation.
It often starts subtly. You might notice that birds don’t seem to chirp as loudly as they used to, or the “S” and “T” sounds in conversation seem to disappear when you’re watching the evening news. Maybe you find yourself nodding along at dinner parties—not because you heard what was said, but because you don’t want to ask your friend to repeat themselves for the third time.
If this sounds familiar, you aren’t alone, and you aren’t imagining things. You may be experiencing presbycusis.
While the medical term might sound intimidating, presbycusis is simply the scientific name for age-related hearing loss. This guide explores what presbycusis is, why it happens, how it affects daily life, and how you can manage it to stay connected to the world around you.
What Is Presbycusis?
To understand the condition, it helps to look at the word itself. The term comes from the Greek words presbys (meaning “old” or “elder”) and akousis (meaning “hearing”). Put simply, presbycusis is the gradual loss of hearing in both ears that commonly occurs as we age.
While you might see the term “presbycusis disease” used in medical literature or billing codes, it can be more helpful to think of it less as a disease and more as a natural, cumulative process. Just as our eyesight changes and we eventually need reading glasses (a condition called presbyopia), our auditory system also changes over time.

How Presbycusis Differs from Other Hearing Loss
Presbycusis is different from other types of hearing impairment. Unlike noise-induced hearing loss (which can happen suddenly after an explosion, gunshot, or loud event—or gradually from long-term exposure to loud machinery), presbycusis is almost always:
- Sensorineural: It affects the inner ear or the auditory nerve, not the outer or middle ear.
- Bilateral: It typically affects both ears in a similar way.
- Gradual: The changes happen slowly, so you may not realize your hearing has diminished until someone else points it out.
- Permanent: Because it involves the degradation of nerve cells and hair cells, it cannot be medically “cured” or reversed—but it can be effectively treated and managed.
The Scope of the Issue
If you have been diagnosed with presbycusis, you are in good company. Research suggests that:
- Roughly 1 in 3 adults between the ages of 65 and 74 has some hearing loss.
- Among people older than 75, nearly half experience hearing loss.
Acknowledging the condition is the first step toward a better quality of life. The biggest mistake people make is assuming that hearing loss is an inevitable decline that must be endured in silence. Modern hearing care proves otherwise.
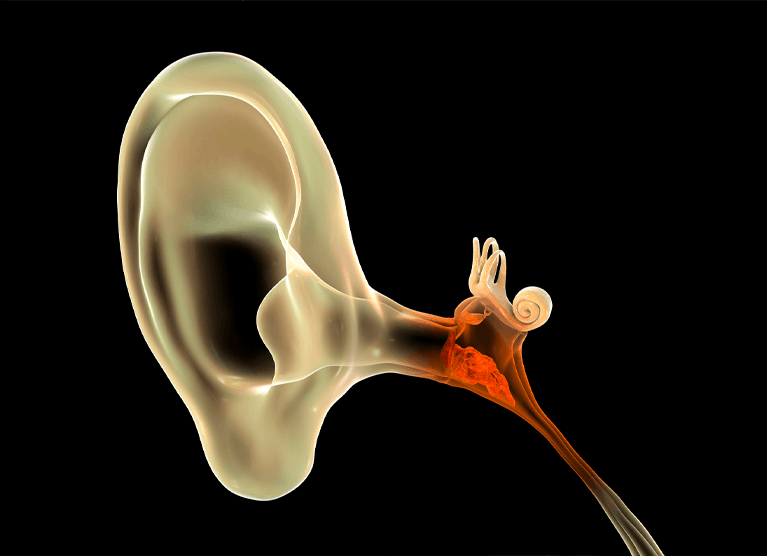
The Biology of Listening: What Causes Presbycusis?
To understand why presbycusis happens, we need to look inside the inner ear—specifically at a snail-shaped structure called the cochlea.
Inside the cochlea are thousands of tiny, microscopic hair cells. These aren’t like the hairs you see on your arms; they are specialized sensory receptors. When sound waves enter your ear, they cause fluid inside the cochlea to ripple, bending these hair cells. This bending creates electrical signals that travel up the auditory nerve to the brain. Your brain then interprets those signals as sound—music, traffic, or a loved one’s voice.
The “Wear and Tear” Effect
Presbycusis is largely the result of lifetime wear and tear on these delicate structures:
- Hair cell damage: Over decades, hair cells can become damaged or die. Unlike skin cells, inner-ear hair cells do not regenerate. Once they are gone, they are gone.
- Nerve degeneration: The pathways that carry signals from the ear to the brain can weaken over time.
- Reduced blood supply: Changes in blood flow to the ear can impact the health of the cochlea.
Why High Frequencies Go First
You might notice you can hear a truck rumbling past your house (a low-frequency sound) perfectly well, but struggle to hear the timer on your microwave or the high-pitched voices of children.
This is a classic hallmark of presbycusis. The hair cells located at the base of the cochlea—the ones responsible for detecting high-pitched sounds—are the most fragile and typically the first to wear out. This is why women’s and children’s voices often become difficult to understand before lower-pitched voices do.

The Four Main Types of Presbycusis
While the overall outcome is hearing loss, researchers have categorized presbycusis into four main types, depending on which part of the auditory system is primarily affected. Most people experience a combination rather than just one.
1. Sensory Presbycusis
Caused by the loss of sensory hair cells at the basal (high-frequency) end of the cochlea.
The result: A sharp drop-off in high-frequency hearing. Speech discrimination (understanding words) is often relatively preserved in quiet settings if the volume is high enough, though clarity in background noise may still be difficult.
2. Neural Presbycusis
Involves degeneration of the nerve cells in the cochlea and central auditory pathways.
The result: The ability to understand speech is significantly worse than what the audiogram alone might suggest. Even when sounds are amplified, the signal reaching the brain is distorted. This is sometimes described as phonemic regression.
3. Metabolic (Strial) Presbycusis
Related to changes in the stria vascularis, a tissue that maintains the chemical balance and blood supply in the cochlea.
The result: A relatively “flat” hearing loss, meaning reduced hearing across low, mid, and high frequencies. This pattern often runs in families.
4. Mechanical (Cochlear Conductive) Presbycusis
Occurs when the physical structures of the cochlea—especially the basilar membrane—become stiffer and less flexible.
The result: A gradual, sloping hearing loss where high notes are harder to hear than low notes, though not as sharply as in sensory presbycusis.

Recognizing the Signs: What Does Presbycusis Feel Like?
Presbycusis doesn’t usually hurt, which is part of why it can go unnoticed for years. Instead, it shows up as a series of communication and everyday listening challenges.
The “Cocktail Party” Effect
The most common complaint isn’t that the world is too quiet—it’s that the world is too muddy. You may hear the volume of a conversation, but the clarity is missing.
In noisy environments like restaurants or parties, picking out one voice becomes exhausting. Background noise drowns out the consonants (such as p, k, f, s, th) that give speech meaning.
Common Symptoms Include:
- Muffled speech: People sound like they’re mumbling or speaking with a hand over their mouth.
- Difficulty with phones: Voices on the telephone can sound tinny, faint, or unclear.
- “Volume wars” at home: You need the TV or radio turned up much louder than others prefer.
- Tinnitus: Ringing, buzzing, or hissing sounds in one or both ears often accompany age-related hearing loss.
- Sound sensitivity: While you can’t hear soft sounds, loud sounds may feel uncomfortably loud or even painful (a condition called recruitment).
The Emotional Toll
Untreated presbycusis can lead to emotional and social strain. Because your brain has to work harder to “fill in the blanks” of what you miss, you may experience:
- Listening fatigue: Feeling drained after conversations or social events.
- Social withdrawal: Avoiding parties, restaurants, or phone calls because listening is tiring or embarrassing.
- Misunderstandings: Answering incorrectly or missing jokes and comments, which can affect confidence and relationships.

Causes and Risk Factors: “Why Me?”
While aging is the primary driver, it’s not the only factor. Two people the same age can have very different hearing, often due to a combination of genetics and life experiences.
1. Genetics
Just as you inherit your eye color, you may inherit a tendency toward earlier or more pronounced hearing changes. If your parents or grandparents had age-related hearing loss, your risk is higher.
2. Noise Exposure
Your lifetime noise history matters. You may be at higher risk if you:
- Worked in loud environments (factories, construction, military service, aviation, etc.)
- Used loud tools or machinery without hearing protection
- Frequently attended loud concerts or listened to high-volume music
This is technically noise-induced hearing loss, but it often compounds with presbycusis as you age.
3. Medical Conditions
Conditions that affect blood flow and overall health can speed up cochlear deterioration, including:
- High blood pressure (hypertension)
- Diabetes
- Heart disease
- Peripheral vascular disease or poor circulation
4. Ototoxic Medications
Certain medications can be toxic to the inner ear (ototoxic), especially with long-term use or high doses. Examples include:
- Some antibiotics
- Certain chemotherapy drugs (e.g., cisplatin)
- High doses or prolonged use of aspirin and some NSAIDs
These medications may accelerate or worsen age-related hearing loss. Never stop a prescribed medication without speaking with your doctor, but do mention any new hearing changes right away.

Diagnosis: What to Expect at a Hearing Checkup
If you suspect presbycusis, the first step is a comprehensive hearing evaluation. The process is painless, non-invasive, and extremely informative.
1. Physical Exam (Otoscopy)
A hearing care professional will look into your ears with a lighted instrument called an otoscope to check for:
- Earwax buildup (cerumen impaction)
- Fluid, infection, or damage to the eardrum
- Other visible issues in the ear canal
Sometimes what feels like permanent hearing loss is actually a simple blockage that can be treated quickly.
2. Pure-Tone Audiometry
This is the familiar “beep” test. You’ll sit in a sound-treated booth wearing headphones. The hearing care professional will play tones at different pitches and volumes, and you’ll indicate when you hear them.
The results create an audiogram, a graph showing your hearing thresholds at various frequencies. A classic presbycusis audiogram shows a sloping pattern—hearing is relatively better for low frequencies and declines as pitch gets higher.
3. Speech Audiometry
Because many people with presbycusis say, “I can hear, but I can’t understand,” speech testing is essential.
- Speech Reception Threshold (SRT): The softest level at which you can repeat simple words.
- Word Recognition Score (WRS): You listen to words at a comfortable loudness and repeat them back, measuring how clearly your brain understands speech when volume isn’t the main issue.
These results help determine how much benefit you’re likely to get from hearing aids and what types of technology or strategies will help most.
Treatment and Management: Reclaiming Your Hearing
Can presbycusis be cured? Currently, the answer is no. We can’t yet regrow damaged hair cells or nerve fibers in the inner ear.
However, presbycusis can be managed very effectively. The goal is to maximize your remaining hearing, keep your brain engaged with sound, and support your quality of life.
1. Hearing Aids
Hearing aids are the gold standard treatment for presbycusis. Today’s devices are sophisticated, discreet, and highly customizable.
Key benefits include:
- Digital processing: They don’t simply make everything louder; they selectively amplify the frequencies you have trouble hearing (often high pitches) while keeping other sounds balanced.
- Noise reduction: Advanced algorithms help separate speech from background noise, making conversations clearer in real-world settings.
- Connectivity: Many models stream phone calls, TV audio, and music directly from smartphones or accessories via Bluetooth.
- Variety of styles: From receiver-in-ear (RIE) models that sit discreetly behind the ear to nearly invisible in-the-canal devices, there are options to match your preferences and hearing needs.
2. Cochlear Implants
For severe to profound presbycusis, where hearing aids are no longer sufficient, cochlear implants may be considered. Unlike hearing aids, cochlear implants bypass damaged parts of the inner ear and directly stimulate the auditory nerve.
Eligibility is determined through specialized testing by an implant team (usually including an ENT surgeon and an audiologist).
3. Assistive Listening Devices (ALDs)
ALDs can complement hearing aids or, in some situations, provide additional support:
- TV streamers: Send TV audio directly to your hearing aids or headphones so you don’t have to turn the volume up for everyone.
- Captioned telephones: Display written text of what the caller is saying.
- Personal amplifiers (pocket talkers): Use a microphone and headphones to boost a specific speaker’s voice, useful in hospitals or one-on-one conversations.
4. Communication Strategies
Technology works best when paired with simple behavioral strategies:
- Use visual cues: Face the person speaking and ask them to face you. Lip movements and facial expressions help fill in what your ears miss.
- Improve the environment: Reduce background noise (turn off the TV, move away from loud vents), and sit closer to the speaker.
- Advocate for yourself: Let others know you have hearing loss and suggest what helps, such as speaking a bit more slowly or saying your name before starting to talk.

Prevention: Protecting the Hearing You Have
You can’t stop the clock on aging, but you can help prevent your hearing from worsening faster than necessary.
Protect your ears:
- Wear earplugs or earmuffs when exposed to loud sounds (concerts, power tools, lawnmowers, hunting, etc.).
- Avoid prolonged use of headphones at high volumes—follow the “60/60 rule” (no more than 60% volume for 60 minutes at a time).
Support overall health:
- Manage blood pressure, blood sugar, and cholesterol with your provider’s guidance.
- Stay physically active and maintain a heart-healthy lifestyle.
- Follow a balanced diet that includes nutrients important for vascular and nerve health.
Taking the Next Step
Presbycusis is a common part of aging for many people—but it does not have to define your later years. The isolation that often comes from untreated hearing loss is optional.
If you recognize signs in yourself or a loved one—muffled TV, difficulty in restaurants, ringing in the ears—don’t wait. The earlier you address hearing loss, the easier it is for your brain to adapt to hearing aids and the better your long-term cognitive and social health will be.
Make an appointment with a hearing care professional to discuss your concerns, get a baseline hearing check, and explore your options. It’s not just about hearing better; it’s about fully engaging with the people and moments that matter most.
Key Takeaways
- Presbycusis is the medical term for age-related, sensorineural hearing loss.
- It usually affects high frequencies first, impacting clarity more than volume.
- It is caused by gradual changes in the inner ear and auditory pathways.
- Tinnitus (ringing in the ears) commonly occurs alongside presbycusis.
- There is no cure, but hearing aids and communication strategies offer excellent management options.
Frequently Asked Questions
A sudden loss of hearing is a medical emergency that's different from presbycusis. If this happens, seek immediate medical attention.
If you have more questions, don't hesitate to talk to your healthcare provider or a hearing care professional. Knowledge and early action are key to staying tuned in to life's conversations and moments.
Sources and Additional Learning
- American Academy of Audiology, “Seniors and Hearing Loss” – https://www.audiology.org/consumers-and-patients/seniors-hearing-loss/
- American Speech-Language-Hearing Association, “Hearing Loss in Adults” – https://www.asha.org/practice-portal/clinical-topics/hearing-loss/
- Center for Hearing and Communication, “The Facts About Hearing Loss” – https://www.chchearing.org/facts-about-hearing-loss
- Cleveland Clinic, “Presbycusis (Age-Related Hearing Loss)” – https://my.clevelandclinic.org/health/diseases/5840-age-related-hearing-loss
- Hearing Loss Association of America, “Hearing Loss: Signs, Symptoms and Steps” – https://www.hearingloss.org/understanding-hearing-loss/hearing-loss-101/signs-symptoms-and-steps/
- Johns Hopkins Medicine, “Age-Related Hearing Loss (Presbycusis)” – https://www.hopkinsmedicine.org/health/conditions-and-diseases/presbycusis
- Mayo Clinic, “Hearing Loss” – https://www.mayoclinic.org/diseases-conditions/hearing-loss/diagnosis-treatment/drc-20373077
- NIH: National Institute on Deafness and Other Communication Disorders, “Age-Related Hearing Loss (Presbycusis)” – https://www.nidcd.nih.gov/health/age-related-hearing-loss
- NIH: National Institute on Deafness and Other Communication Disorders, “Hearing Aids” – https://www.nidcd.nih.gov/health/hearing-aids
- NIH: National Library of Medicine, “Presbycusis” – https://www.ncbi.nlm.nih.gov/books/NBK559220/
- WHO: World Report on Hearing 2021 – https://www.who.int/publications/i/item/9789240020481
Note: This article is for educational purposes only and is not medical advice. If you are experiencing sudden hearing loss in one or both ears, seek immediate medical attention, as this is a medical emergency different from presbycusis.

Take Online Hearing Test
Take our free at-home hearing loss test as a first step on your journey to better hearing.

Book Your Free Appointment

Reviewed By
MJ DeSousa; B.Sc.(H), M.Cl.Sc, Aud(C)
MJ DeSousa is an Audiologist and Director of Patient Experience at Beltone, with over 35 years of experience in hearing health care. She earned her Masters of Clinical Science in Audiology from Western University in London, Ontario and has extensive experience as a practicing Audiologist and in corporate leadership within the hearing industry. At Beltone, DeSousa is dedicated to educating hearing care professionals across North America, ensuring they provide the highest standard of patient care. Learn more by visiting her LinkedIn here.

Reviewed By
Kathy McGowan, AuD CCC-A, Doctor of Audiology
Kathy McGowan is the Manager of Managed Care Programs with Beltone Corporation . Kathy worked with the Professional Development Training Team as well as the Operations Team and Beltone Corporate Retail for 8 years before being promoted to her current position. Prior to joining Beltone Corporate, Kathy worked for 10 years as an Audiology Manager in a private practice. She has worked in many settings as an Audiologist including an ENT practice, a hospital, an Optical and Hearing Company, and in the Military, retiring as a LtCol. Kathy earned her Bachelor’s in Speech and Hearing and Master’s in Audiology from Ohio University in Athens, Ohio, and went on to receive her Audiology Doctorate from A.T. Still University School of Health Sciences. Kathy is currently licensed in seven states.

